Percutaneous Coronary Intervention (PCI)
Why is a Percutaneous Coronary Intervention (PCI) done?
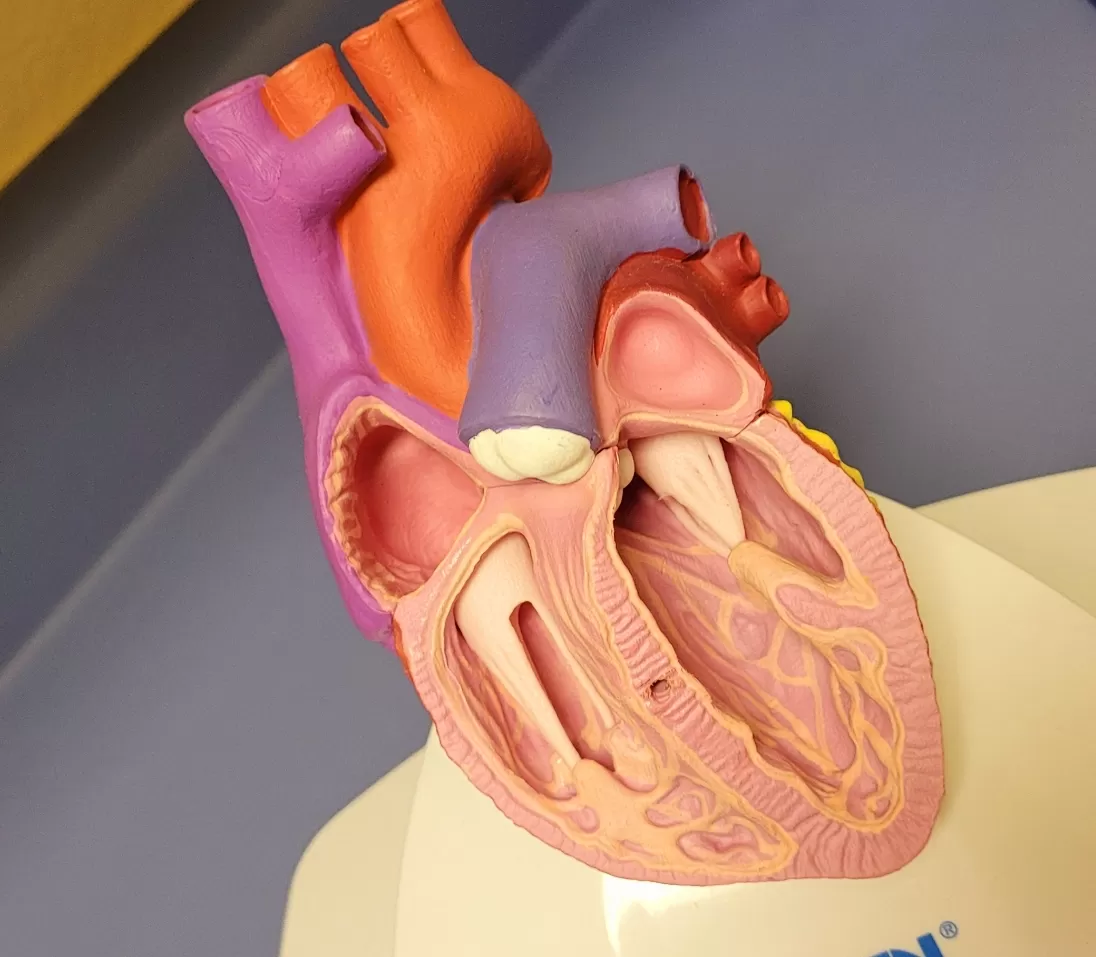
The coronary arteries supply the heart muscle with blood that contains oxygen. The heart needs oxygen to pump blood around your body.
A narrowing or blockage in a coronary artery can cause symptoms such as chest pain or heaviness.
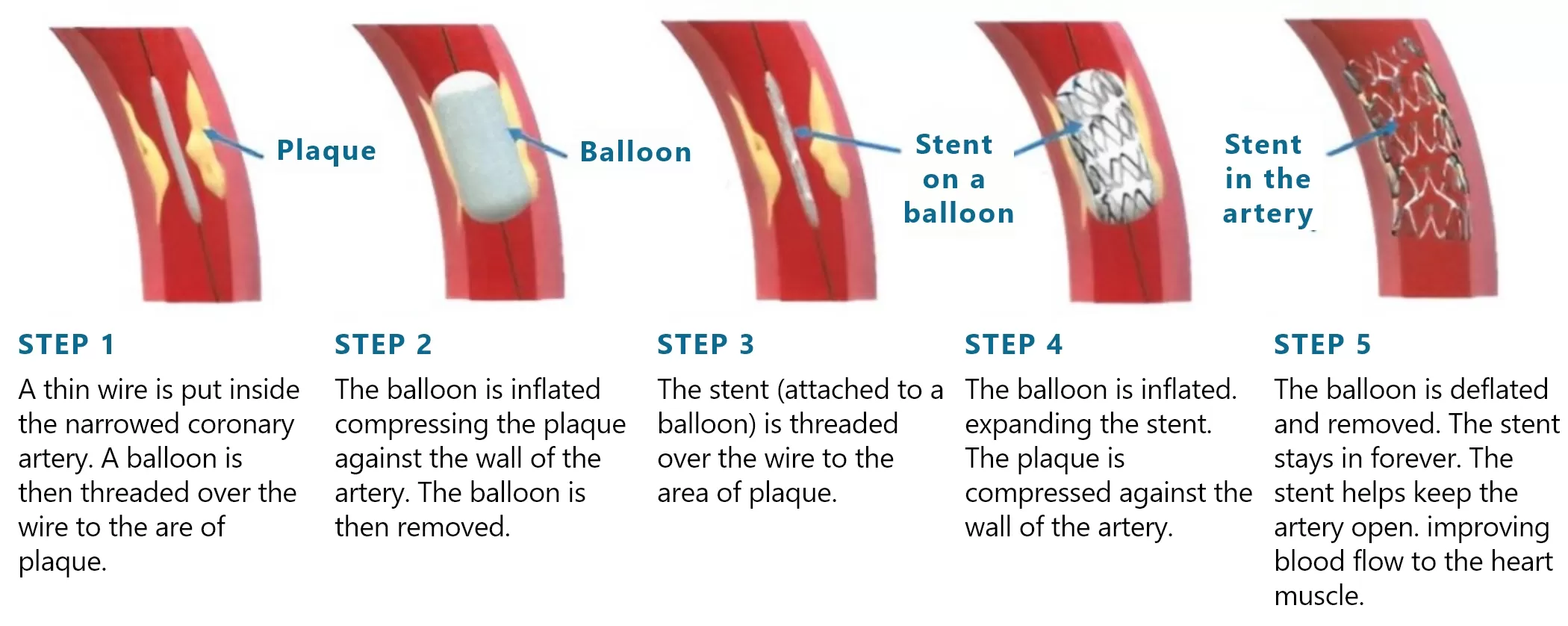
What is a PCI Procedure?
A balloon angioplasty is normally performed (steps 1 &2) before a stent is inserted (steps 3, 4 & 5). A stent is a metal mesh tube that holds back the plaque that has caused your artery to narrow or block.
How long does the procedure take?
A PCI normallv takes about 45 minutes to 1 hour.
What are the risks?
Your doctor has recommended you for a percutaneous coronary intervention (PCI) as they believe the benefits to you outweigh the risk of not going ahead with the procedure. There are risks and complications related to this procedure. They include but are not limited to the following:
Minor or major bruising or swelling at the puncture site.
Narrowing or blockage of the coronary artery again. Different factors can affect this and your doctor will discuss these with you.
Loss of pulse in the limb used for the procedure afterwards.
Heart attack.
Abnormal heart rhythm that may need an electric shock to correct.
Surgical repair of the groin/arm puncture site or blood vessel.
A stroke. This can cause long term disability.
Loss of kidney function due to the side effects of the contrast dye.
A higher lifetime risk of cancer from x-ray exposure.
Rupture of a blood vessel that needs emergency surgery/heart surgery or a blood transfusion to fix.
A reaction to the x-ray dye or blood thinning medications.
Blockage of the stent within the first month of the procedure. This may need another PCI or surgery to fix.
Death as a result of this procedure is rare.
Before Your Procedure
Do not eat anything 6 hours before your procedure, you may drink only clear fluids up until 2 hours before your procedure.
If you take Metformin (Diabex®, Diaformin®) stop taking 2 days before and 2 days after your procedure.
If you take Empagliflozin (Glyxambi®, Jardiamet®, Jardiance®) or Dapagliflozin (Forxiga®, Xigduo XR®, Qtern®) stop taking 3 days before.
Please let us know if you are allergic to lodine, Contrast or any other medications.
Your Cardiologist may stop your Warfarin, Dabigatran (Pradaxa®), Rivaroxaban (Xarelto®) & Apixaban (Eliquis®) 2-3 days before the procedure.
Aspirin, Clopidogrel (Plavix®), Ticagrelor (Brilinta®) and Prasugrel (Effient®) need to be continued.
Ask any questions that you or your family may have and sign a form consenting to the procedure.
Please arrange a friend or family member to take you home from hospital and stay with you for your first night at home. You cannot go home alone or in a taxi.
You will change into a hospital gown, an ID band applied
Your procedure site (groin and wrist) clipped of any hair. The healthcare team will take your blood pressure and pulse and insert an IV (intravenous) line into a vein in your arm.
During the Procedure
Your PCI is done in a Cardiac Catheterisation Laboratory (Cath Lab). It is a sterile lab and the staff will be wearing gowns, masks and caps.
You will lie flat on your back on a narrow x-ray table.
Your groin and/or wrist will be cleaned with a cold antiseptic solution and then you will be covered with a drape. It is important that you try and stay still under the drape.
A heart tracing is placed on your chest for the whole procedure.
After the local anaesthetic is injected, your groin or wrist will become numb and the procedure will begin.
After the Procedure
The catheters (tubes) will be removed and the incision closed by pressing on the site, use
of a stitch/plug or by placing a band around your wrist to apply pressure. Your doctor will explain the results of the procedure and recommend the best treatment for you. You will return to the ward where you will stay until you are discharged.
Activity After the Procedure & At Home
Rest on the day of your procedure in a bed or recliner chair.
Avoid strenuous activity such as mowing, running or hard labour and do not lift objects more than 5kg (10lbs) for 5 days afterwards. Slowly return to normal activities the next day.
Limit stair climbing as much as possible on the day of your procedure.
Limit the use of the affected limb for the next 48 hours such as eating with that arm, using a phone, typing, bending or squatting.

Blood Thinning Medications After the Procedure
Your doctor will prescribe blood-thinning medicines (antiplatelet) to help prevent blood clots. The medicine include: o Aspirin o Clopidogrel (Plavix®), Ticagrelor (Brilinta®) or Prasugrel (Effient®).
Do not stop taking these medications without talking to your Cardiologist.
Please make sure you have these medications before you leave the hospital.
Driving once you are home
Do not drive for 2 days after your procedure.
If you have had a heart attack or drive a commercial vehicle you may not be able to drive for 2-4 weeks.
More information can be found from your Cardiologist or the Roads and Maritime Services.
Follow Up
Please see your local doctor in 3 days and make an appointment to see you Cardiologist within 4 weeks.
Wound Site Care
The dressing on your wrist or groin can be removed the day after your procedure.
You may take a shower the day after your procedure, do not take a bath or go swimming for 2 days after your procedure. Do not scrub the wound site for a week, lightly wash and pat dry. Avoid creams, lotions or ointments to the wound site.
Notify your nurse or doctor if you notice any of the following:
A lump that is getting bigger or any swelling at the procedure site
Constant redness or warmth
Worsening numbness or discomfort (mild discomfort is normal)
Yellow ooze/pus from the wound site

If there is bleeding or a lump getting bigger at the wound site
1) Lie down straight away and apply firm pressure (enough to feel the heart beat under your fingers) to the site for 15 minutes.
2) If bleeding continues or is a large uncontrolled amount or you feel faint or dizzy call ‘000’ immediately. Do not drive yourself to the hospital. Continue to apply pressure until help arrives.
What To Do If You Experience Any Chest Discomfort
If it is travelling to your shoulder, arm, neck or jaw, crushing weight or pressure and combined with any sweating, shortness of breath, nausea or fear.
At the first sign of discomfort
Stop immediately and rest
If no relief with rest
Take 1st nitroglycerine (GTN) tablet or spray
If no relief within 5 minutes
Take 2nd nitroglycerine (GTN) tablet or spray
If no relief after 5 minutes
Call an ambulance ‘000’ and take 3rd nitroglycerine (GTN) tablet or spray
Notify your GP or Cardiologist you have any pain that is relieved by nitroglycerine (GTN) tablet or spray.
** GTN belongs to a group of medicines called nitrates. It lets more blood and oxygen reach the heart muscle.

